|
|
|
|
|
| |
Quality general dental care with an emphasis on natural esthetics, form and function. Experience with complex restorative, prosthetic and implant treatment.
----------------------------------------------------------------------------------------
OCCLUSION AND YOUR BITE
Occlusion, means simply the contact between teeth when the patient brings their jaws together. More technically, it is the relationship between the maxillary (upper) and mandibular (lower) teeth when they approach each other, as occurs during chewing or at rest.
Malocclusion is the misalignment of teeth and jaws, or more simply, a "bad bite". Malocclusion can cause number of health and dental problems.
Static occlusion refers to contact between teeth when the jaw is closed and stationary, while dynamic occlusion refers to occlusal contacts made when the jaw is moving, as with chewing.
Centric occlusion is the occlusion of opposing teeth when the mandible is in centric relation. Centric occlusion is the first tooth contact and may or may not coincide with maximum intercuspation. It is also referred to as a person's habitual bite, bite of convenience, or intercuspation position (ICP). Centric relation, not to be confused with centric occlusion, is a relationship between the upper and lower jaw.
Occlusal problems
Malocclusion can cause a number of problems, not just with teeth, but with the supporting bone and surrounding soft (gum) tissue, the temporomandibular joint (TMJ), and jaw muscles. Teeth, fillings, and crowns may wear, break, or loosen, and teeth may be tender or ache. Receding gums can be exacerbated by a faulty bite. TMJ problems, broadly termed temporomandibular joint disorder or TMJ syndrome, can include clicking, grinding, or pain in the jaw joint, ringing or buzzing in the ears, and difficulty opening and closing the mouth. If the jaw is malpositioned, jaw muscles may have to work harder, which can lead to fatigue and or muscle spasms. This in turn can lead to headaches or migraines, eye or sinus pain, and pain in the neck, shoulder, or even back. Untreated damaging malocclusion can lead to occlusal trauma which can lead to loosening of the teeth, excessive wear of the teeth and drifting of the teeth into new positions.
Some of the treatments for different occlusal problems include tooth adjustments, replacement of teeth, medication (usually temporary), a diet of softer foods, and relaxation therapy for stress-related clenching. Fixed appliances, known as orthodontics or dental braces, may be used to adjust the occlusion, and removable appliances, called occlusal splints, may be used to alleviate pain in the TMJ, prevent further damage and wear of the teeth and supporting structures.
But how does the mouth work from an occlusion standpoint? The anterior teeth protect the posterior teeth by providing for a plane of guidance during excursions, thus allowing the cusps of the posterior teeth to disclude rather than strike one another during lateral or protrusive movements from centric relation. In other words, the posterior teeth have much larger crowns and many more cusps than the anterior teeth. Because posterior crowns are so much wider and possess cuspal projections in various configurations, the cusps of the maxillary teeth and those of the mandibular teeth have an opportunity to bang into each other during chewing, speech or simply meeting together when one bites down. To prevent this from happening, the anterior teeth of each arch will, ideally, be situated so as to come into contact before the cusps of the posterior teeth do, thus averting such a situation.
The posterior teeth protect the anterior teeth by providing a stable vertical dimension of occlusion. While anterior teeth may retain their natural position even after loss of posterior teeth, the masticatory forces will eventually cause the single-rooted anterior to splay, thus leading to a collapsed bite.
Occlusal splints (also called bite splints, bite planes, or night guards) are removable dental appliances carefully molded to custom fit the upper or lower arches of teeth of a patient.
They are used to protect teeth/implants and restoration surfaces, manage mandibular (jaw) dysfunction, and stabilize occlusion or create space prior to restoration procedures. Patients prone to nocturnal bruxism (nighttime clenching or grinding), should routinely wear occlusal splints at night to take stress of the TMJ and its a associated muscles and prevent damage to the teeth/implants and associated bone and soft (gum) tissue.
Occlusal splints are typically made of acrylic resin. There are several types of splints and these may be hard, soft or combination of hard and soft materials. Soft splints have a tendency to cause “rebound” chewing in patients and are not as durable as hard splints. Hard splints are more durable and stable, but are not as comfortable to wear for some patients as soft splints. Splints made of a combination hard soft material offer the best of both worlds. They are durable as the exterior in contact with the opposing teeth is hard and they are more comfortable as the interior secures it to the teeth in the arch is soft.
The splint generally covers all the teeth of the upper or lower arch, but partial coverage is sometimes used. Occlusal splints are usually used on either the upper or the lower teeth, termed maxillary splints or mandibular splints respectively. We favor mandibular (lower) splints as they are less likely to interfere with speech and can be worn during the day without being obvious like a maxillary (upper) splint.
Pankey-type occlusal splints are “flat-plane” with a flat surface against the opposing teeth, and help jaw muscle relaxation, while repositioning occlusal splints are used to reposition the jaw to improve occlusion. These are used when chronic pain in the joint is present and allows the joints to find a comfortable position. These may be used early in full mouth construction also to determine the best position to restore the mouth to.
Tanner-type occlusal splints have depressions in the surface that the opposing teeth contact providing positive contacts. These type splints are used for patients who are showing wear of the teeth or damage to the supporting bone and soft tissue. Additionally, they are used to protect teeth and implants in those patients who clench their teeth and may be of benefit to those who exercise as most patients clench during exercise.
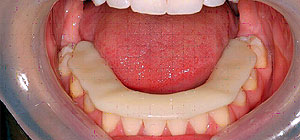
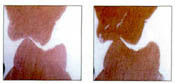
Occlusal splint on the lower arch
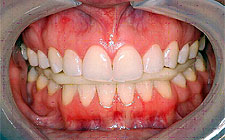
Patient biting with an occlusal splint in the lower arch
Pankey splint
The Pankey Splint is a flat plane splint made from a tooth colored acrylic resin material. The occlusal scheme is created with one point occlusal contact per posterior tooth, combined with anterior and cuspid guidance. This allows for total posterior disclusion in all excursions. The Pankey splint is used in patients with: acute pain in the temporomandibular joint (TMJ), chronic issues with the TMJ and when the dentist is trying to determine where the joint and teeth need to be have the joint in Centric Relation (CR) to allow a starting point for restoration of the mouth. This is basically a deprogrammer appliance as there is no locked position for the posterior cusps so the joint will settle into a comfortable position without moving into the habitual positions. Typically this type appliance is worn 24/7 except when eating to allow the joint to become deprogrammed. Occlusal adjustments are made every few days after initial insertion to maintain the even point contacts then this moves to weekly then biweekly until a stable position is achieved.
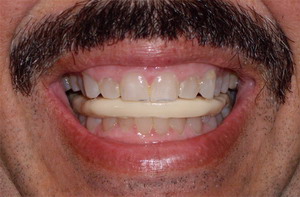 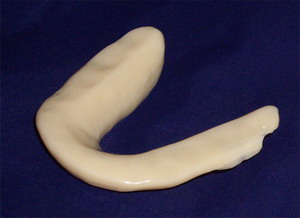
Patient wearing the Pankey splint and teeth occluded and the splint out of the mouth demonstrating the flat plane design.
Tanner Splint
The Tanner Splint is similar to the Pankey splint except that the surface that the opposing teeth will contact has indentations for the cusps of the teeth it is also made from a tooth colored acrylic resin material. The occlusal scheme is created with wide indentations for the posterior teeth to be able to move through all functional motions and is combined with anterior and cuspid guidance. This allows for total posterior disclusion in all excursions. The Tanner splint is used in patients with: chronic pain in the TMJ, patients who are nocturnal clenchers and bruxer’s (grind their teeth) and as a long term stabilizer appliance to prevent damage to teeth and dental restorations. Patients who wear Tanner splints may wish to wear while exercising to prevent clenching during activity.
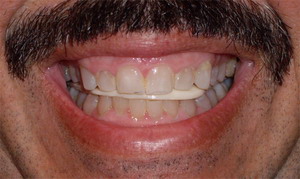 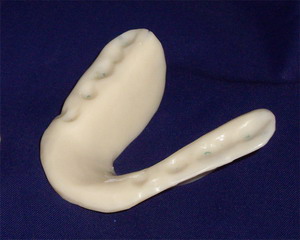
Patient wearing the Tanner splint and teeth occluded and the splint out of the mouth demonstrating the occlusal indented design.
Dental Compression Syndrome
- Fear
- Anger
- Dreaming
- Medical
- Sleep Apnea
- Pain in other parts of the body
- Dental
- Teeth not closing together comfortably
Since thirty percent of the people who clench and grind their teeth are not aware they're doing it, it's important that the signs of this disorder be recognized during routine visits to the dentist, or through self-examination.
(Information provided courtesy of Dr. Gene McCoy for further information please email him at gmccoydds@aol.com or visit his website at www.toothcrunch.com)
Dental Compression Syndrome (DCS) is a contemporary name for the centuries-old bad habit of compressing and grinding one's teeth.
The damage that occurs can be devastating to the component structures of the mouth. The force of compression and grinding, which can easily exceed 500 lbs. per square inch, simultaneously applies pressure to the teeth, to the bone supporting the teeth, and to the temporomandibular joint (TMJ), where the mandible (lower jaw) hinges with the skull.
These heavy repetitive load applications, over a period of time, can cause headaches, facial pain, neck and shoulder pain, supporting bone loss, sensitive teeth, fractured teeth, ringing in the ears, dizziness, and problems concerning the TMJ.
Approximately ninety percent of the population exhibits damage from DCS, but few are aware of the condition, because this habit tends to be subconscious.
Why do people clench and grind their teeth?
Ninety percent of the time the answer is life stress. But there are other possible reasons, and all contributing factors need to be considered for proper management.
The following is a list of causes that must be considered:
- Exercise and Sports
- Water-skiing
- Weight Lifting
- Motorcycling
- Stimulants
- Amphetamines
- Cocaine
- Caffeine
- Ecstasy
- Psychological
- Anxiety
- Stress
- Fear
- Anger
- Dreaming
- Medical
- Sleep Apnea
- Pain in other parts of the body
- Dental
- Teeth not closing together comfortably
Since thirty percent of the people who clench and grind their teeth are not aware they're doing it, it's important that the signs of this disorder be recognized during routine visits to the dentist, or through self-examination.
What should you look for?
- Overall Appearance
Enlarged muscles on the sides of the face
- Soft Tissue Changes
Receding tissue around the necks of the teeth
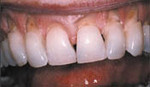
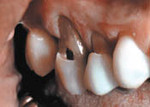
- Dentition
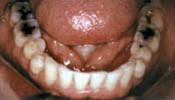
Flattened posterior teeth
Shortened front teeth
Dulling of the tips of the cuspids
Perfectly formed dimples in the biting (occlusal) surface of the posterior teeth
Wedge-shaped defects usually found at the necks of the teeth.
- Bone
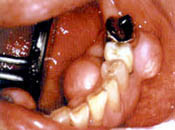
While bone around a tooth may deteriorate due to the excessive pressure of DCS, the opposite effect can also occur.
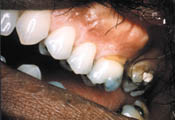
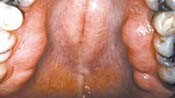
It is not unusual to see areas of bony projections form under the tongue, on the roof of the mouth, or around the roots of teeth.
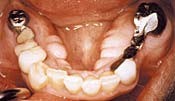
The reason this happens is because teeth and bone are composed of collagen, which when compressed due to DCS creates an electric (piezoelectric) effect, which in turn stimulates bone growth.
- Occlusal Dimples
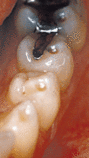
These Highly Polished appearance of these unique cavications may be due to the positive ions emitted from focal points of high stress
Equilibriation: How the teeth fit together
When your teeth do touch, how exactly are they touching? Is it in a comfortable manner, or is it uncomfortable? Equilibration can easily be tested at the dentist's office by placing thin strips of green wax on the teeth and closing once.
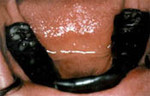
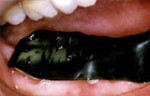
The impressions in the wax are then carefully examined. Ideal contacts are those confined to the tips of the cusps. Heavy contacts are minimized by sharpening or reshaping the teeth. The procedure is simple, does not hurt, and only a minute amount of enamel is removed.
Nature's Ideal Contact
How long does it take?
Although a thirty-minute appointment is reserved for the procedure, it only takes about ten to fifteen minutes to re-contour the teeth, and then there is a short follow-up appointment for "fine tuning."
What does it feel like afterwards?
It is hard to explain because the patient is feeling less stress on the teeth. That is because they are fitting together and feeling better. The sharpening procedure reduces the physical stress where the root of the tooth enters the cone, which is exactly what we want.
Evaluating the benefits:
- The teeth are never shortened
- Physical stress at the necks of teeth is reduced
- The mandible returns to its natural position
- Chewing efficiency improves
- Less force is required to chew
- The tendency to compress the teeth is reduced
- Stress on bone supporting the teeth is reduced
- Stress on the TMJ is reduced
Does the sharpening procedure eliminate the tendency to clench ones teeth?
Only if that is the sole reason one is clenching. In other words, many patients are uncomfortable because their teeth do not fit together properly, and unconsciously squeeze their teeth together in order to make the problem go away, but it only gets worse. If their teeth are more comfortable when they close, the tendency to clench goes away, or greatly diminishes.
However, this does not mean that the psychological component goes away. The sharpening procedure takes care of the engineering component, but we also have to be concerned with the psychological or stress component. For this, the patient needs to wear some sort of guard to protect his or her teeth and TMJ during periods of unconscious clenching.
“The Truth about Occlusion” (link to the PDF)
Implant Cosmetic Dental Center™
----------------------------------------------------------------------------------------
Dr. Gregori M. Kurtzman is an international lecturer, selected as one of the top 100 dental speakers since 2006 by Dentistry Today, author of over 200 professional articles, a consultant to multiple dental manufacturers for product evaluation, development and research, he provides general dental care in suburban Maryland since 1986.
|
|
|
|
|
|
|
|
|